Placental abruption
What is the placenta?
The placenta is an organ that helps your baby grow and develop. It’s attached to the lining of the womb and is connected to your baby by the umbilical cord. The placenta passes oxygen, nutrients and antibodies from your blood supply to your baby.
What is a placental abruption?
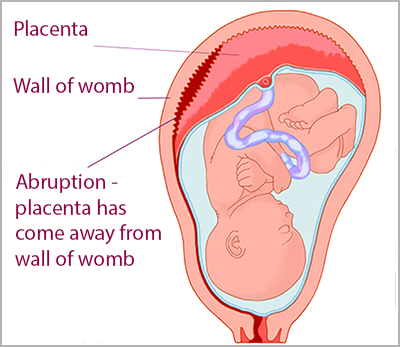
A placental abruption is when some, or all, of the placenta separates from the wall of the womb (uterus) before the baby is born.
A placental abruption may lead to pregnancy complications. How serious these are will depend on how severe the abruption is and how far along you are in your pregnancy.
Placental abruption increases the risk of your baby being born prematurely. It may also affect your baby’s growth. Sadly, a very small number of babies do not survive placental abruption and may be stillborn.
This sounds scary. But the important thing to focus on is taking care of yourself as best you can during your pregnancy. And if you have any symptoms that concern you, your healthcare team will do everything they can to keep you and your baby safe.
Placental abruption affects up to 1 in 100 (1%) of pregnancies.
What are the symptoms of placental abruption?
Placental abruption usually happens in the second half of pregnancy. But it’s important to get checked out if you have these symptoms at any point in your pregnancy.
Vaginal bleeding
Most people with placental abruption have vaginal bleeding. Even though this is the most common symptom of placental abruption, not everyone will have this. So it’s important to get help if you have any other symptoms, even if you are not bleeding.
Abdominal (stomach) pain
Abdominal (stomach) pain or cramping is another common symptom of placental abruption. The level of pain with an abruption can vary. Some women feel as if their tummy is bruised, while others describe the pain as very severe or even excruciating.
Contractions
Some people start having contractions or their bump may feel tense or hard.
Lower back pain
Some people have lower back pain. This may happen if there is a concealed abruption. This is where the blood is behind the placenta, so you won’t have any vaginal bleeding.
If you are concerned about your symptoms
If you feel that something is wrong, or if you are worried about your baby, it’s important to get medical advice. Do not worry if you've talked about it before – you’re not wasting anyone’s time.
Speak to your midwife, GP, or local maternity unit straight away if you think you have symptoms of a placental abruption. If you are unable to contact them, call 111 for advice.
Call 999 if you have severe bleeding or pain that is making you feel very unwell.
What causes a placental abruption?
Doctors do not always know exactly why placental abruption happens, but there are some things that may increase the risk.
Smoking
Smoking can double the risk of having a placental abruption. Quitting smoking can be difficult but there is lots of help and support out there for you.
If your partner or anyone else who lives with you smokes, their smoke can also affect you and your baby before and after their birth. They should understand the risks and try to stop smoking too.
Trauma
An injury to the abdominal area (stomach), such as a car accident, a serious fall or domestic violence, can increase the risk of placental abruption. Speak to your midwife, GP, or local maternity unit straight away if you have any type of injury to the stomach.
Other causes
There is also strong evidence that placental abruption is more likely if you:
- have chronic high blood pressure
- have pre-eclampsia
- use cocaine
- have an intrauterine infection
- have a uterine abnormality
- have had a placental abruption before
- have too little amniotic fluid (oligohydramnios).
There is also some evidence that placental abruption is more likely if:
- you have had a c-section before
- your waters break early (PPROM) during pregnancy
- this is not your first baby
- you are over 40 years old
- you are carrying more than 1 baby.
How is placental abruption diagnosed?
If your healthcare professional thinks you may have a placental abruption, they will ask you about your symptoms, any risk factors and your pregnancy history.
You will also have an internal examination and your baby’s heart rate will be monitored. You may also have an ultrasound.
What happens if I have a placental abruption?
Your treatment will depend on how many weeks pregnant you are, how well you and your baby are and how severe the abruption is.
If you are near your due date (more than 34 weeks pregnant), you will be recommended to give birth straight away. You may be able to delivery vaginally, but if you or your baby are not well you may be recommended to have an caesarean section.
If you are less than 34 weeks pregnant, the abruption is small, and you and your baby are well, your doctor may recommend that they monitor you and your baby closely for the rest of your pregnancy. This will give your baby more time to develop before being born.
Monitoring may include regular ultrasound scans, fetal heart rate monitoring and other tests. These are to make sure that you and your baby stay well. You may be advised to stay in hospital during this time.
You may be recommended to give birth by 37 to 38 weeks. This is to reduce the risk of stillbirth.
If you are less than 34 weeks pregnant and you or your baby are very unwell, you may need to give birth immediately by emergency c-section.
This can be scary, but you will be cared for by a specialist team with expertise in offering the care that you need.
Can I do anything to prevent placental abruption?
We don’t know for sure what causes placental abruption, so there is nothing you can do to guarantee it won’t happen. But there are some things you can do to reduce your risk:
- Go to all your antenatal appointments. This will help make sure you and your unborn baby are as well as possible throughout your pregnancy.
- Avoid any intensive or high-impact sports. Your midwife can give your more advice.
- If you are a smoker, get help to give up smoking.
- Do not take illegal or recreational drugs in pregnancy. Cocaine, in particular, can increase your risk of placental abruption.
- Domestic abuse can happen to anyone. You may feel trapped and that there is no way out but there is lots of help available. We have more information about domestic abuse. If you're worried someone might see you have visited this page, the Women's Aid website tells you how to cover your tracks online.
Getting pregnant again
If you’ve had a placental abruption before, there is an increased risk that it may happen again. But this does not mean it will.
Your midwife or doctor will probably monitor your other pregnancies very carefully. You can also do things to prevent placental abruption, such as stopping smoking.
BMJ Best Practice (2022) Placental abruption. https://bestpractice.bmj.com/topics/en-gb/1117
Tikkanen, M. (2011), Placental abruption: epidemiology, risk factors and consequences. Acta Obstetricia et Gynecologica Scandinavica, 90: 140-149: https://obgyn.onlinelibrary.wiley.com/doi/full/10.1111/j.1600-0412.2010.01030.x
NHS. Stop smoking in pregnancy. https://www.nhs.uk/pregnancy/keeping-well/stop-smoking/ (Page last reviewed: 7 November 2019 Next review due: 7 November 2022)

