A dad’s journey through NICU
https://www.tommys.org/Tommy’s blog by James Farina
Having a baby preterm can be an anxious experience that comes with a number challenges, for you and your baby.
Being born too soon can mean your baby might be underdeveloped, small and potentially very poorly.
Often preterm babies are taken away to the neonatal intensive care unit (NICU) for any medical attention they may need.
Whilst we know that this separation is hard to manage, the baby unit is the best place for your little one if they are unwell.
Mothers of premature babies may experience various emotions after birth, such as anxiety, grief or guilt.
Kaleena Berryman, mother to premature baby Jharid, said;
'The baby was growing in my womb, so who else could I blame?'
Dads sometimes get overlooked, but it is important to remember that preterm birth is difficult for them too.
It can be hard to juggle the needs of their partner, visit their baby in NICU and manage their own emotions.
James Farina was confronted with the realities of premature birth when his partner Lucy began experiencing tight pains at 24+5 weeks.
Here is James’ journey through NICU
At the end of September 2015, we discovered that we were going to have a baby. On the first scan we were given a due date of 28th June.
15 weeks into the pregnancy, I was woken up by loud bangs in the bathroom. Lucy had passed out; her eyes had rolled to the back of her head and her body was stiff and shaking. All I could do was hold her close to stop her from hurting herself.
We went to the hospital for a check-up but they couldn’t find any issues so we went home to rest.
From that moment on Lucy was constantly feeling poorly with terrible headaches, lack of energy and a horrible feeling that things were just not right. Despite visiting the doctor and midwife on several occasions, nobody could work out what was going on.
On the 13th March 2016, only 24 weeks and 5 days (24+5) into pregnancy, Lucy started to get some tight pains which we thought were Braxton Hicks contractions.
The following day Lucy woke me up at four in the morning in a lot of pain saying we needed to go to the hospital. The doctor did an internal exam and they noticed the membranes were bulging and Lucy was already 3cm dilated.
It’s at this point that things got very real very fast. We were told that there was a very high chance of going into labour within the next few hours.
This was due to a possible infection of the uterus and the body’s natural defence is to get the baby out.
Lucy was given a steroid injection in her leg to help with the baby’s lungs. Lucy was then wheeled in to the delivery room on a bed and hooked up to a drip that delivered magnesium sulphate into the blood to help protect the baby’s brain, which made Lucy feel quite “funny”.
On one of her visits to the toilet her waters broke so I called in the nurse. The doctor came in to do a scan on Lucy and noticed the waters had gone and there was no longer any cervix so the baby was definitely on its way.
Lucy’s contractions were quite irregular at around 8-25 minutes apart but they were getting much stronger. We were made fully aware of what we should expect in the coming hours. We were told of the chances of survival and possible health issues for the baby.
I knew I should have been thinking positively but all I could think was that our journey as parents could come to an end very shortly.
The baby’s heart beat was starting to slow down which was a huge concern. Seconds later a team of doctors walked in and set up the incubator and monitors in the corner of the room.
Lucy was told that on her next contraction she must push as hard as possible otherwise the chance of survival would be greatly reduced for the baby.
At this point, after going through a million different emotions, knowing Lucy was unwell and the baby was fighting for its life I felt the most helpless I’ve ever felt in my life.
The only thing I was able to do was stand by Lucy and hold her hand but the main thing was to not get in the doctor’s way!
When the baby arrived, it was the most surreal moment of my life.
One part of me was happy that I’d just become a father but the other part of me was scared because the baby was lifeless and I thought the worst.
I didn’t know if our baby was a girl or boy or even if they were alive. Our baby was quickly taken to the other side of the room where the team of doctors worked hard to clear the airways, keep the baby warm and try to save the baby’s life.
I then hear one of them say “She’s breathing“. These were the most incredible words I’ve ever heard.
In those 2 words I found out that our baby was alive and that we had a daughter. I’ll never forget that moment. Lucy asked me if she heard right and I replied saying I think so.
She then cried and jokingly asked if she was ginger. I said “No she’s got brown hair.” and Lucy did a celebratory fist punch showing that even after everything Lucy had been through, she still had her sense of humour.
Lucy saw our daughter and quickly gave her a kiss before she was taken down to NICU (Neonatal Intensive Care Unit) and I went with her.
She didn’t look human and I didn’t feel like I was a father, she was so tiny and red with her eyelids still fused together. I could see all of her veins; she was just skin and bones.
She looked like she was fighting for her life and I thought she could go at any time. There was literally nothing I could do to help. I felt love for her instantly and was staring at her for ages.
One of the nurses came up to me and started talking to me about my daughter. She was very kind and knew exactly how to talk to me which was reassuring.
I was told that she weighed 700 grams (1lbs 8oz) and briefly told what was going on inside the incubator. The doctors then had to do some tests so I left and went back to Lucy.
After waiting a couple of hours in the delivery room, we were both allowed to go and see our daughter together.
I wheeled Lucy down on a wheelchair into NICU, we went over to the incubator and we both looked in. I could tell it was a big shock for Lucy.
We could only stay there for a few minutes before we headed back up to the delivery room. Soon after, we had a name for her; Robyn May Farina.
We would read to Robyn every day and just before we left, we would put a blanket over the incubator, away from all of the flashing lights and monitors to keep it as dark and calm as possible.
Over the next few days Robyn had a blue light above the incubator to help with jaundice. This was taken away once her skin started to improve.
Her eyes started to open too which was incredible to see. They were completely black for a while but they slowly started to turn a gorgeous bright blue.
Whilst in the incubator, she grabbed our fingers which was amazing; such a strong grip for such a tiny baby.
A valve in Robyn’s heart was still open at this point. This would usually close before birth but it hadn’t had time to yet. In order to move things along the doctors would give Robyn very small doses of Ibuprofen.
She also needed Sytron to help with her iron levels and needed a couple of blood transfusions.
For the first 7 days we were only able to touch her through the incubator doors but every 7 days the baby’s incubator gets changed.
Just before this was done we were asked by a nurse if we’d like to hold her for the first time. We, of course, said yes!
They took her out; at this point she was covered with tubes and wires and looked half machine. We were both quite scared but so excited. Lucy sat in a recliner chair, they wrapped Robyn up in some warm blankets and Lucy held her.
After many photos she was passed to me. We felt like real parents for the first time! Robyn would occasionally open her eyes. She couldn’t see properly yet but she’d look towards our voices so I think she recognised us.
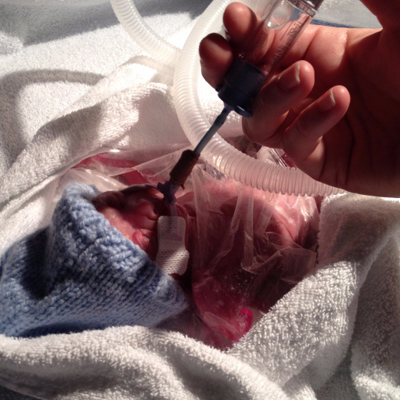
Almost straight away Lucy was asked to express milk. Robyn started on a tiny 0.7ml of milk every three hours. She was fed via a tube which went through her mouth down into her stomach.
We were eventually allowed to feed her ourselves after being shown how to. We learnt a huge amount whilst in NICU.
Changing her nappy was an interesting one! We had to put our arms through the incubator doors and navigate countless wires and tubes and used sterilised water with cotton balls. We did this whenever we were there and it helped us feel like parents that little bit more.
Robyn started off in the intensive care unit (ITU), and then eventually when she started to improve she’d move rooms.
Each room she’d move to would be a room for less dependent babies and less machines. She’d go from ITU to High Dependency 1 (HD1) then to Special Care 1 (SC1) and finally to SC2.
On one occasion she went back a room after a bad turn, this was very worrying for us both but it wasn’t long until she recovered.
Thankfully, we knew that Robyn was in the very best place possible.
The doctors were absolutely incredible. They were so kind, easy to talk to and obviously incredibly good at their jobs. Lights would constantly be going off with babies having desats and brady’s but the doctors would sort it out promptly and calmly without panic.
We would only ever leave Robyn’s side to go home once she was stable and resting. This was for our own peace of mind too.
We knew that she’d have desaturations when we weren’t in the room though and this was a difficult thing to think about but we had to keep thinking of the positives and her progress.
After a while we were able to hold her on a regular basis and started to do kangaroo care. This was skin to skin contact holding; incredible for bonding with each other.
When Robyn was ready, Lucy was able to breastfeed which was amazing. Lucy felt more like a mother every time which was lovely to see and eventually Robyn’s feeding tube could be removed and she’d only be bottle and breastfed.
Near to the end of our NICU journey we were invited twice to stay overnight in a private room with Robyn in a cot next to us. At this point she was still on oxygen. This was great but we had a very sleepless night. We were constantly checking on her.
There were no nurses with us but they were only a corridor away and we had a panic button in case of any problems. Luckily we didn’t need any help and we fed and changed her completely on our own while keeping an eye on her monitors.
Days later her ECG leads would eventually be taken away. Her feed and weight would increase. Her assisted oxygen would reduce. Her eyes and ears would be tested and results came back great, she’d move from an incubator to a heated cot and finally to an unheated cot with no support from any machine.
Robyn had 2 overnight traces which would show the doctors exactly how Robyn was doing and how close she was to being allowed to go home.
The first trace came back and showed a couple of big desats so she wasn’t quite ready yet. The second overnight trace a few days later proved to be very good.
In order to come home she had to have a good overnight trace, 3 good eye tests and be solely on bottle and breast feeding. She would have been allowed to leave on home oxygen, but fortunately for us, Robyn was now breathing completely on her own so there was no need for this.
We also had a baby first aid training session at the hospital before leaving and that’s something we felt was so important to have.
Just before we could take Robyn home, we had a discharge planning meeting with the doctor. She talked about how important it was that we protect her from germs that are harmless to us but could have an incredibly bad effect on Robyn while still vulnerable.
As soon as we all went home and went outdoors we found it a very hard and frustrating challenge to stop random people from reaching in the pram so we designed a badge which simply says,
“Please don’t touch me, I’ve been very poorly.”
This worked so well that it inspired us to set up a small business called BubbahBear for premature baby care products for babies and their parents.
We also recently became supporters of Tommy’s to give something back to their incredible charity. They specialise in providing research into premature birth and they also do a lot of support and advice for parents.
Having a child in NICU will shape your life for the foreseeable future. For myself and my fiancée Lucy, this experience was the hardest, most emotional, testing and stressful time of our lives but at the same time, we became stronger and I wouldn’t change a thing.
More information
The best thing you can do for your baby is to look after yourself. That way, you will be better equipped to handle the challenges that face you and your family. Here are our practical tips for surviving the baby unit and early days after premature birth.
Having a premature baby is a huge adjustment and it may take you a long time to accept what has happened. Here is our advice on adjusting to your new reality after premature birth.
If you want to read more from James you can take a look at his blog, a Dad’s NICU Journey.
Read more stories about premature birth
-
Read more about 'This experience made us and our son stronger 'Premature birth blogs
This experience made us and our son stronger
-
Read more about 'Born Too Soon; a poem about preterm birth 'Premature birth blogs
Born Too Soon; a poem about preterm birth
-
Read more about 'What we can learn from parents of premature babies 'Premature birth blogs
What we can learn from parents of premature babies
-
Read more about 'Looking back, I’m glad that Professor Quenby was so cautious 'Premature birth blogs
Looking back, I’m glad that Professor Quenby was so cautious
